Participant Support Procedures > Dysphagia Support Procedure
Authorised by Chief Executive Officer
Approved date: 19 September 2023
Statement
Kyeema is committed to ensure workers delivering high intensity dysphagia support meet the needs of each participant. Kyeema ensures the workers are aware of and understand the relevant health support plan. The dysphagia health support plan has been developed and is overseen by a speech pathologist, and each participant is involved in the assessment and development of their health support plan (HSP). The support plan is up to date, reviewed annually, readily available, clear, and concise and clearly identifies and describes the support needs and preferences of the participant.
Kyeema will determine whether the participant is to initially receive dysphagia supports or mealtime management. This decision will involve the participant and health practitioners.
This procedure supports Kyeema to apply the NDIS practice standards Module 1 – High Intensity Daily Personal Activities Module
Scope
This procedure applies to relevant managers, participants and the workers who support participants with high intensity daily personal activities.
Relevant legislation
NDIS Practice Standards
NDIS Practice Standards: High Intensity Support Skill Descriptors current version
Definitions
Dysphagia support: participants with severe dysphagia are at a higher risk of choking and aspiration and may need more specialised supports to eat and drink safely.
Mealtime management: Participants who can participate in mealtimes with minimal assistance may only need mealtime management supports.
Choking: is a life-threatening emergency that occurs when an object blocks the airway, preventing breathing.
Aspiration: the process of inhaling food, liquid, or other material into the lungs. Aspiration is a common problem in people with dysphagia.
IDDSI Framework: The IDDSI framework consists of a continuum of 8 levels (0 - 7), where drinks are measured from Levels 0 – 4, while foods are measured from Levels 3 – 7. The IDDSI Framework provides a common terminology to describe food textures and drink thickness.
Mealtime management only or mealtime management with dysphagia supports
Dysphagia supports are for participants with severe dysphagia. They are assessed by a speech pathologist, require a mealtime management plan, and are supported by workers trained in high intensity dysphagia supports.
Participants with only mealtime management support can participate in mealtimes with minimal assistance and are not at risk of choking or aspiration. They are assessed by a health practitioner, require a mealtime management plan, and are supported by workers with general training in mealtime management.
If unsure whether a participant needs dysphagia supports or mealtime management supports, consult with a speech pathologist. The speech pathologist will assess the participants swallowing difficulty and make recommendations for the type of supports they need. The specific supports will vary depending on the individual’s needs.
The participants goals and preferences are important to consider when determining the type of supports they need. Some participants may be willing to accept a certain level of risk to eat and drink independently, while others may prefer more assistance to minimise the risk of choking.
Each participant will be categorised as needing either mealtime management or dysphagia supports on:
•the health practitioners support plan or CCF-83 Mealtime Management or Dysphagia Support
Procedure
Before supporting a participant with high intensity needs, the worker is required to:
•agree to and sign their own Individual Training Plan (ITP)
•attend all training requirements as per their ITP
•read and understand the participants Health Support Plan – Mealtime Management or Dysphagia Support CCF-83 or the relevant health practitioners care plan
•after reading the health support plan or care plan, sign and date the Staff Acknowledgement – Health Support Plans CCF-59, kept in the participants file
The procedure for dysphagia supports is different from the procedure for mealtime management. Dysphagia supports are specifically designed to help people with swallowing difficulties. Mealtime management is the general process of providing assistance with eating and drinking.
Mealtime management procedure:
Refer to the mealtime management procedure on Kyeema’s QMS for the detailed procedure.
1. Assess the participants needs - identify the participants level of independence, their ability to participate in mealtimes, their goals and preferences.
2. Participants who are identified as needing assistance with meals are referred to a speech therapist or qualified practitioner for assessment.
3. Plan the mealtime supports - determine the specific supports that the participant needs, such as assistance with cutting food, feeding and positioning (use the IDDSI framework)
4. Implementing the mealtime supports – provide the participant with the necessary assistance during mealtimes.
5. Evaluate the effectiveness of the supports – monitor the participants progress and adjust the supports needed.
Dysphagia supports procedure:
1. Assess the participants swallowing difficulty – this involves a speech pathologist conducting a swallowing assessment to determine the nature of the severity of swallowing.
2. The speech pathologist develops the mealtime plan –they will base the plan on the results of the swallowing assessment and should include specific recommendations for modifying food textures, positioning and other aspects of mealtimes (use the IDDSI framework).
3. Implement the severe dysphagia health support plan – provide the participant with the necessary assistance in accordance with the plan.
4. Position the participant correctly – the participant should be positioned in a way that minimises the risk of choking or aspiration. This may mean sitting upright, tilting the head forward, or using a chin tuck manoeuvre.
5. Feed the participant slowly and carefully, giving them time to chew and swallow each bite.
6. Be alert for signs of choking and respond with first aid if needed.
7. Clean up spills immediately to prevent the participant from aspirating food or liquid.
8. Evaluate the effectiveness of the plan – monitor the participants progress at every meal. Support workers to document mealtime on Carelink shift notes and report any issues to their supervisor.
9. The dysphagia support plan will be reviewed annually by a speech pathologist.
Ensuring the participants safety
This is the most important priority, and it is important to take steps to minimise the risk of choking or aspiration:
•Follow the speech pathologist’s health support plan
•Choose appropriate food textures - Follow the IDDSI Framework
•Follow food safety procedures
•Avoid distractions during mealtimes
•Discourage talking whilst eating and drinking
•Do not force the person to eat or drink
•Offer small bites and sips
•Allow the participant to take their time
•Respect the participants dignity and independence
Respecting the participants dignity and independence.
The participant should be involved in the planning and implementation of the supports, and they should be given as much independence as possible.
Dysphagia symptoms include:
•difficulty biting or chewing on food
•coughing or choking on food or fluid
•food or drink falling from a person’s mouth.
These can worsen as people age.
Risks associated with dysphagia
People with disability, who have dysphagia, are more likely to die from choking or respiratory illnesses (or have serious health complications).
A regular comprehensive health assessment can help to identify health issues earlier.
Managing risks
An accurate assessment of a participant’s swallowing and nutritional needs can reduce the negative impacts of dysphagia and improve their safety and quality of life.
If Kyeema workers notice participants that are struggling with swallowing food or fluids, the worker will notify the team leader. The team leader will notify the family and request for a speech pathologist to review the participants mealtime management plan. If the participant does not have a mealtime management plan a request for an assessment by a speech pathologist will be made.
Refusal to share or follow their dysphagia plan
When the participant refuses to share or follow their mealtime management plan, Kyeema will seek documentation from a health practitioner or other; stating that they refuse to share or follow their dysphagia plan. Kyeema workers will continue to monitor, report, and strive to provide a safe environment for the participant under these circumstances.
Making mealtimes enjoyable
Mealtimes should be a positive experience for the participant, and they should be encouraged to participate as much as possible. It is important for the worker to be understanding, patient and compassionate. Mealtimes can be challenging for people with dysphagia and the worker should do their best to make the experience as positive as possible.
Oral health
Support the participant to maintain oral health. Follow the health practitioners care plan for oral health. Alternatively check with the health practitioner if the following steps can be used for the participant.
Steps to support the participant to maintain oral health:
•Brush their teeth at least twice daily with toothpaste and a soft brush.
•Use a bought mouthwash or home-made salt solution
(1 teaspoon salt added to 1 litre of water) as needed to freshen the mouth and breath.
Report any bleeding or mouth problems to the supervisor / health practitioner.
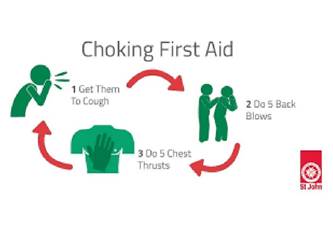
Emergency actions:
1. Stay calm and breathe.
2. If the participant is choking completely (can’t speak), call 000
3. Administer first aid (workers have current First Aid and CPR training)
4. Call supervisor

Reporting incidents
•Write up the shift notes during the shift, not at home in your personal time
•Report incidents to your team leader/supervisor/supports manager and document in the shift notes
•Your supervisor may request an incident report form to be filled out
•In an emergency call 000 and /or your supervisor
Awareness & Training
In addition to the general training (First Aid & CPR, food safety, infection control), workers will be trained in the specific needs of each participant they support. Training should be delivered by an appropriately qualified health practitioner such as a speech pathologist.
Kyeema should ensure that workers understand the support needs outlined in the support plan and what risks to look for and actions required to respond to risks, incidents, and emergencies.
Workers are required to complete a skills review (recommended annually) and participate in participant specific training with a health practitioner. The training officer and/or supports manager will let workers know when this will occur.
Where a worker has not delivered this support for a period of more than three months, or if a participant’s support needs have changed and/or they have an updated support plan in place, it is recommended the worker be reassessed before supporting the participant and undertake refresher training if required.
Training provided:
Individual training plan (ITP)
•K:\Admin\Training\High Intensity Supports ITP\Individual Training Plan
Participant specific training with a healthcare professional and the worker/s
•Participant Specific Training Attendance Sheet HRF- 46
•K:\Admin\Training – Participant Specific Training HISW
Sentrient online training:
•Complex Care – Advanced Mealtime Management
•Complex Care – Mealtime Refresher (annual)
•Comple Care – Severe Dysphagia Management
•Complex Care – Severe Dysphagia Management Refresher (annual refresher)
•HISW – Dysphagia – Modified Food & Fluids Poster IDDSI
Form used for workers to reflect and identify gaps in skills and knowledge:
•High Intensity Supports Skills review – Severe Dysphagia CCF-54
Responsibilities
The training officer will organise training for the workers.
The training officer will email a monthly reminder to team leaders to communicate any staffing and health plan changes.
The training officer and supports manager are responsible for ensuring workers have current skills and knowledge, and that the training of workers is documented and regularly audited.
•High Intensity Supports Skills review – Severe Dysphagia CCF-54
The team leader is responsible for supporting the participant to seek annual reviews of their severe dysphagia health support plan. Mealtime management plans are to be reviewed annually by a speech pathologist or qualified health practitioner. If the plan is unchanged, the team leader will add the revised date to the current plan stating that the plan is unchanged.
•Health Support Plan – Mealtime Management or Dysphagia Support CCF-83 or the health practitioners support plan
The team leader is responsible for communicating any staffing and health plan changes to the training officer.
The team leader is responsible for notifying the training officer of new mealtime management or dysphagia support plans as per the speech pathologist.
The support worker is responsible for attending all allocated training sessions.
Support workers are responsible for reporting any changes to the participants dysphagia supports, participants health and wellbeing to their supervisor.
The support workers is responsible for reading, understanding, and signing the participants HSP:
•Staff Acknowledgement – Health Support Plans CCF-59 or the acknowledgement attached to the HSP.
Review and Evaluation
Mealtime management plans are to be reviewed annually by the health practitioner. If the plan is unchanged, the team leader will add the revised date to the plan stating that the plan is unchanged. The worker supports the participant to provide feedback and request changes to their support plan as required.
Record Keeping
Hard copies are filed in workers and participant files.
Electronic records are kept in participants file, Sentrient and the k/d spreadsheet.
•Individual Training Plan K:\Admin\Training\High Intensity Supports ITP\Individual Training Plan
•High Intensity participant specific training (working document) K:\Admin\Training – Participant Specific Training HISW
Related Documents
NDIS Practice Standards: High Intensity Support Skill Descriptors current version
Practice Alert: Dysphagia, safe swallowing & mealtime management
Health Support Plan – Mealtime Management or Dysphagia Support CCF-83
High Intensity Supports Skills review – Severe Dysphagia CCF-54
Staff Acknowledgement – Health Support Plans CCF-59
Participant Specific Training Attendance Sheet HRF-46
High Intensity Supports Procedure
Incident Reporting Policy and Procedure