Participant Support Procedures > Enteral Feeding Support Procedure
Authorised by Chief Executive Officer
Approved date: 12 September 2023
Statement
Kyeema is committed to ensure workers delivering enteral feeding support meet the needs of each participant. Kyeema ensures the workers are aware of and understand the relevant health support plan. The support plan for enteral feeding and management has been developed and is overseen by a relevant health practitioner (may involve more than one health practitioner e.g. dietician, speech therapist, occupational therapist), and each participant is involved in the assessment and development of their support plan. The support plan is up-to-date, readily available, clear and concise and clearly identifies and describes the support needs and preferences of the participant.
This procedure supports Kyeema to apply the NDIS practice standards Module 1 – High Intensity Daily Personal Activities Module
Scope
This procedure applies to relevant managers, participants and the workers who support participants with high intensity daily personal activities.
Relevant legislation
NDIS Practice Standards
NDIS Practice Standards: High Intensity Support Skill Descriptors current version.
Definitions
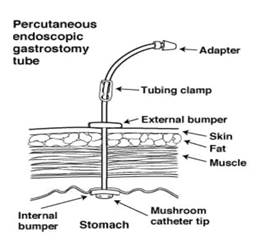
Percutaneous endoscopic gastrostomy (PEG) is a procedure to place a feeding tube. These feeding tubes are often called PEG tubes or G tubes. The tube allows you to receive nutrition directly through your stomach. This type of feeding is also known as enteral feeding or enteral nutrition.

Enteral feeding stoma site is the location on the abdomen where a feeding tube is inserted into the body.
Procedure
Before supporting a participant with high intensity needs, the worker is required to:
•agree to and sign their own Individual Training Plan (ITP)
•attend all training requirements as per their ITP
•read and understand the participants Health Support Plan – Enteral Feeding CCF-49 or the relevant health practitioners care plan
•after reading the health support plan or care plan, sign and date the Staff Acknowledgement – Health Support Plans CCF-59, kept in the participants file
Consent
The participant must provide their express consent for tube feeding. This must occur prior to the specific procedure being performed for the participant. A participant's consent is not required in emergency situations. For example, where a participant's life is at risk, medical treatment or first aid can be provided even though the participant may not have given consent. In such situations, a shift note setting out the emergency circumstances and the treatment that was carried out is placed on Carelink and reported to your supervisor.
SUPPORT PROCEDURE FOR PEG FEEDING
A mealtime preparation and delivery plan are developed and overseen by a health practitioner e.g., dietician, speech pathologist, occupational therapist. Always refer to the health practitioners care plan first.
Implement the support plan
•Check with the participant for any specific factors or adjustments needed and to confirm they are ready for their meal
•Follows hygiene and infection control procedures and safe food handling, for example, hand washing, use of gloves and disinfecting the environment
•Deliver support in ways that are least intrusive or restrictive and fit into the participant’s daily routines and preferences
•Supports the participant to position themselves for feeding and checks they are ready for their meal
Workers are to wash their hands thoroughly, before using the feeding tubes and equipment.
•The feeding process is not a sterile environment, but it requires very high hygiene standards. It is not a requirement that workers wear gloves, but individual workers may choose to do so
•It is important to ensure the connection is clean and free from any leftover contents. To ensure this, wash tube out under running water, and then syringe through the tube, hot water
•Ensure the correct position of the feeding tube before feeds start
•Store the connection and plastic syringe, on a dish, in the fridge between use (if syringe is used)
•The feeding bag and tubing are disposed of, after each feeding session.
•Double bag the feeding tube before disposal in bin
•The connection and plastic bottle are kept and will be used for at least 3 months.
Correct feeding position
•Never give feeds while lying flat
•Sit in a chair or lie with your head raised to at least 30 degrees or on three pillows. Try to remain in this elevated position after feeding e.g. for 30-60 minutes after a feed.
Steps for Feeding
1. Wash hands thoroughly with soap and water
2. Gather all the necessary equipment, including the feeding tube, feeding formulae, a syringe, a water pitcher and a towel
3. Check the participants feeding plan to determine type of formulae, amount of formulae and feeding schedule
4. Straighten out the tubing feed
5. Pinch and open the stopper (pinching the tube prevents excess air entering the stomach when the stopper is removed)
6. Connect syringe/gravity drip bag to tube
7. Pour 20mls of lukewarm water into the syringe to check for blockage if needed
8. The water must flow smoothly. This will also moisten the tube so that foods will not stick
9. Tilt syringe/gravity drip bag slightly to let air escape if necessary
10. Fill syringe with feed or use gravity drip bag
11. Hold syringe/gravity drip bag upright to let feed flow into the stomach slowly, by gravity. Raising or lowering the syringe/gravity drip bag will cause the flow to go faster and slower respectively. It is not advisable to have a fast flow as this will distend the stomach quickly and may cause discomfort.
12. Gravity drip bag may have a stand to attach it to
13. After feeding, run 30 – 60 mls lukewarm water through the tube to flush it clear
14. Pinch tube and disconnect syringe/gravity drip bag from tube
15. Close the stopper
16. Rinse and dry syringes and keep in closed container
17. Monitor the participants response
18. Document the amount of feeding formulae administered and any problems or complications
Complete the Enteral PEG Feeding Record Chart CCF-96:
•date
•feed times & feed volume
•observations / issues
•your signature
Contact your supervisor / health carer:
• If you notice redness, pain or swelling, or excess discharge around insertion site
• If the feeding tube moves out of position
• Leakage at the insertion site
Additional tips for support workers who are administering enteral feeding:
•Position the participant comfortable in a sitting or reclining position
•Talk to the participant and provide reassurance during feeding
•Monitor the participants breathing and signs of discomfort during the feeding
•Stop the feeding if the participant experiences any discomfort or difficulty breathing
•Clean and store the feeding equipment properly after each use
Caring for PEG feeding tube
There are different types of feeding tubes. Each type will have its own way it needs to be looked after. Refer to the enteral feeding support plan about the care of the feeding tube such as:
• The correct position of the tube
• How to care for the skin around the feeding tube
• When the feeding tube should be changed
Each participant will have specific care needs. Participant specific training will be provided to workers. If a worker is unsure of any part of the procedure, report this to your supervisor and you may request further training.
How long do PEG tubes last?
PEG tubes can last for months or years. They may clog or wear down over time. If the PEG tube is wearing out, you may notice:
• Bumps on the tube
• Leaking
• Pits or indentations on the tube
If you notice any of these symptoms, report these immediately to your supervisor.
Oral health
Support the participant to maintain oral health. The risks of poor oral health can affect people who rely on enteral feeding. Follow the health practitioners care plan for oral health. Alternatively check with the health practitioner if the following steps can be used for the participant.
Steps to support the participant to maintain oral health:
• Brush their teeth at least twice daily with toothpaste and a soft brush.
• Use a bought mouthwash or home-made salt solution
(1 teaspoon salt added to 1 litre of water) as needed to freshen the mouth and breath.
If they have a dry mouth due to the treatment, use a salt solution mouthwash as bought mouthwashes containing alcohol can make the mouth dryer. Ask your nurse more about their mouth care.
Report any bleeding or mouth problems to the supervisor / health practitioner.
Here are some common complications of enteral feeding:
• Aspiration: this is the accidental entry of food or liquid into the lungs. It can cause pneumonia or other respiratory problems
• Tube blockage: This can occur if the feeding tube becomes clogged with food or formulae. It can be cleared by flushing the tube with water or using a feeding tube cleaning kit.
• Infection: This can occur at the site of the feeding tube insertion or in the digestive tract. It is important to practice good hygiene when handling the feeding tube and formulae.
• Skin breakdown: This can occur at the stoma site if it is not properly cared for
• Diarrhea: This can be caused by several factors, including the type of formulae, the rate of feeding, or the length of time the feeding tube has been in place.
• Constipation: This can be caused by dehydration, the type of formulae, or the rate of feeding.
• The PEG tube comes completely out it will need to be replaced as soon as possible because the tract begins to close within 1-2 hours. Participant needs to get to a hospital.
Reporting Complications:
Support workers are to report any complications to the supervisor/team leader immediately and document them in the shift notes. The team leader or manager will report complications to the participants health care professional for review of the care plan.
Some complications may need to be reported to emergency services eg. tube removal. Call 000 and your supervisor immediately.
Awareness & Training
In addition to general training in a range of different types and methods of enteral feeding, workers will be trained in the specific needs of each participant they support, including their enteral feeding regime and the appropriate use of equipment. Training should be delivered by an appropriately qualified health practitioner or a person who meets the expectations of this skills descriptor.
Kyeema should ensure that workers understand the support needs outlined in the support plan such as: enteral tube feeding supports, the type of feeds, the feeding delivery mechanism, specific mealtime assistance techniques, stoma care, what risks to look for and actions required to respond to risks, incidents, and emergencies
Workers are required to complete a skills review (generally annually) and participate in participant specific training with a health practitioner. The training officer and/or supports manager will let workers know when this will occur.
Where a worker has not delivered this support for a period of more than three months, or if a participant’s support needs have changed and/or they have an updated support plan in place, it is recommended the worker be reassessed before supporting the participant and undertake refresher training if required
Training provided:
• Individual training plan (ITP)
• Sentrient online enteral feeding training
• Participant specific training with a healthcare professional and the worker/s
• Participant Specific Training Attendance Sheet HRF- 46
• High Intensity Supports Skills review – Enteral CCF-55 to identify training needs
Training provided:
Individual training plan (ITP)
• K:\Admin\Training\High Intensity Supports ITP\Individual Training Plan
Participant specific training with a healthcare professional and the worker/s
• Participant Specific Training Attendance Sheet HRF- 46
• K:\Admin\Training – Participant Specific Training HISW
Sentrient online training:
• Complex Care – Enteral Feeding Management (PEG Feeding)
• Complex Care – Enteral Feeding Refresher (annual refresher)
Form used for workers to reflect and identify gaps in skills and knowledge:
• High Intensity Supports Skills review – Enteral CCF-55
Responsibilities
The training officer will organise training for the workers.
The training officer will email a monthly reminder to team leaders to communicate any staffing and health plan changes.
The training officer and supports manager are responsible for ensuring workers have current skills and knowledge, and that the training of workers is documented and regularly audited.
• High Intensity Supports Skills review – Enteral CCF-55
The team leader is responsible for updating the health support plan annually. If the enteral feeding plan is unchanged, the team leader will add the revised date to the plan stating that the plan is unchanged.
• Health Support Plan – Enteral Feeding CCF-49 or the health practitioners care plan
The team leader is responsible for filing CCF-96 on a monthly basis in the participant’s file.
• Enteral Feeding Record Chart CCF-96 or the health practitioners urinary output chart
The team leader is responsible for communicating any staffing and health plan changes to the training officer.
Support workers are responsible for attending all allocated training sessions.
Support workers are responsible for reporting any changes to the participants enteral feeding apparatus, health and wellbeing to their supervisor.
Support workers are responsible for reading, understanding and signing the participants HSP:
• Staff Acknowledgement – Health Support Plans CCF-59
Review and Evaluation
The worker supports the participant to provide feedback and request changes to their support plan as required.
Record Keeping
Hard copies are filed in workers and participant files.
Electronic records are kept in participants file, Sentrient and the k/d spreadsheet.
• Participant Specific Training Attendance Sheet HRF – 46
• Individual Training Plan K:\Admin\Training\High Intensity Supports ITP\Individual Training Plan
• High Intensity Supports Skills review – Enteral CCF-55
• High Intensity participant specific training (working document) K:\Admin\Training – Participant Specific Training HISW
• Sentrient courses
• Health Support Plan – Enteral Feeding CCF-49 or the health practitioners care plan
• Staff Acknowledgement – Health Support Plans CCF-59
Related Documents
NDIS Practice Standards: High Intensity Support Skill Descriptors current version
Health Support Plan – Enteral Feeding CCF-49
Enteral PEG Feeding Record Chart CCF-96
High Intensity Supports Skills review – Enteral CCF-55
Staff Acknowledgement – Health Support Plans CCF-59
Participant Specific Training Attendance Sheet HRF-46
Individual Training Plan template – k/d
High Intensity Supports Procedure
Incident Reporting Policy & Procedure