Urinary Catheter Support Procedure
Participant Support Procedures
> Urinary Catheter Support Procedure
Authorised by Chief Executive Officer
Approved date: 19 October 2023
Statement
Kyeema is committed to ensure workers
delivering urinary catheter support meet the needs of each participant. Kyeema
ensures the workers are aware of and understand the relevant health support
plan. The support plan for urinary catheter support has been developed and is
overseen by a relevant health practitioner, and each participant is involved in
the assessment and development of their health support plan (HSP). The support
plan is up to date, reviewed annually or as needed, readily available, clear and
concise and clearly identifies and describes the support needs and preferences
of the participant.
This procedure supports Kyeema to
apply the NDIS practice standards Module 1 – High Intensity Daily Personal
Activities Module
Scope
This
procedure applies to relevant managers, participants and the workers who support
participants with urinary catheters.
Relevant legislation
NDIS
Practice Standards
NDIS
Practice Standards: High Intensity Support Skill Descriptors current
version
Definitions
Urinary Catheter
Support is the
process of cleaning and maintaining a urinary catheter.
Urinary catheter is a small, flexible tube that is
used to collect urine from the body.
Catheter bag is the container that collects the
urine.
Stoma site is the location where a catheter is
inserted into the body.
In-out / Intermittent catheter
is when a
new catheter is inserted each time you need to
drain urine. It is then immediately removed. This is done at intervals similar
to those at which you would go to the toilet to pass urine. This process may be
referred to as ‘clean intermittent self-catheterisation’ or CISC (performed by a nurse). In some cases, male participants who
are incontinent but not urine retentive may be able to wear a catheter attached
to a condom. Females may wear a wick or similar device (performed by support
workers).
In-dwelling/inserted urinary
catheter (performed by a health practitioner)
is a catheter which is inserted into the bladder, via the urethra
and remains in situ to drain urine.
Suprapubic catheter (performed by a health
practitioner) the catheter accesses the bladder directly through the
abdomen.
Autonomic
dysreflexia can
occur in people with spinal cord injuries above the T6 level. Sudden and
uncontrolled increase in heart rate and blood pressure which can lead to stroke,
heart attack or death. Can be caused by
a full bladder, bowel or skin irritation which the brain cannot
control.
Procedure
Before
supporting a participant with high intensity needs, the worker is required
to:
• agree to and sign their
own Individual Training Plan (ITP)
• attend all training
requirements as per their ITP
• read and understand the
participants Health Support Plan – Catheter Care CCF-50 or the relevant health
practitioners care plan
• after reading the health
support plan or care plan, sign and date the Staff Acknowledgement – Health
Support Plans CCF-59, kept in the participants file
It is
important to follow the specific instructions in the participants support plan
and to consult with the supervisor/health practitioner for
clarification. Before starting the bag
changing procedure, confirm that the support plan is the correct and current
plan for the participant.
CATHETER BAG
PPE
Always
wash hands with warm soapy water, wear eye protection and gloves
when:
• Cleaning around the
catheter site
• Emptying or changing the
urine collection bag
• Connecting/disconnecting
overnight bag
• Cleaning any equipment
used
Steps for changing the catheter bag
You
will need these supplies:
• A clean washcloth or
gauze
• Night bag or leg bag (as
appropriate)
• alcohol pads x
2
1. Wash your hands thoroughly with soap
and water
2. check for the participants consent,
expectations, capacity and preferences for being involved in the delivery of the
support
3. Explain the procedure to the
participant
4. Help the participant to a comfortable
position to change the bag
5. Follow specific procedures listed by
the health practitioner
o Empty the urine from the drainage bag
into the toilet. Make sure that spout of the drainage bag never touches the side
of the toilet or any emptying container.
o Place the clean cloth or gauze under
the connector to catch any leakage.
o Pinch off the catheter with your
fingers and disconnect the used bag.
o Wipe the end of the catheter with an
alcohol pad.
o Wipe the connector on the new bag with
the second alcohol pad.
o Connect the clean bag to the catheter
and release your finger pinch.
o Check all connections. Straighten any
kinks or twists in the tubing.
6. The nurse will insert the urinary
catheter tubing, support workers are required to change the catheter bag as
needed
7. Wash hands thoroughly with soap and
water
8. Measure and record the amount and
consistency of urine on the Urinary Catheter Output Chart CCF-93 or the chart
supplied by the health practitioner
9. Record shift notes on
carelink+
Cleaning the catheter bag:
You
will need these supplies:
• White vinegar
• Cool water
1. Wash your hands thoroughly with soap
and warm water.
2. Rinse the bag with cool water. Don’t
use hot water because it can damage the plastic equipment.
3. To decrease odour, fill the bag
halfway with a mixture of 1-part white vinegar to 3 parts water. Shake the bag
and let it sit for 15 minutes.
4. Rinse the bag with cool water and
hang it up to dry.
Changing the catheter bag: the catheter bag is the container that collects the
urine. It should be changed every 24 hours, or more often if it becomes
full.
Monitoring the catheter: this involves checking the catheter for leaks,
kinks, or blockages. It is also important to monitor the skin around the
catheter for signs of irritation or infection.
Emptying the catheter bag: the catheter bag should be emptied as soon as it
becomes one-third full. This will help to prevent the urine from backing up and
causing infection. Empty the collected urine using a portable urine holder and
flush down the toilet.
Always
fill in the urine record sheet.
Additional tips for catheter care:
• Wash
your hands thoroughly with soap
and water before and after handling the catheter
• Use a clean, dry towel to
wipe the area around the catheter
• Do not use harsh soaps or
antiseptics on the skin around the catheter
• Keep the catheter bag below the level
of the bladder
• Support the participant to
drink plenty of fluids to prevent urinary tract infections
• Report any problems with
the catheter to the supervisor/doctor/health practitioner
It is
important to follow the specific instructions for catheter care that are given
by the doctor/health practitioner. These instructions may vary depending on the
type of catheter and the individual’s needs.
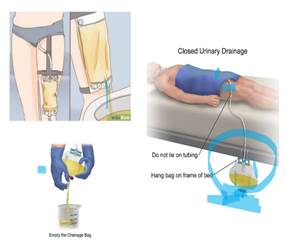
Day
time catheter bag and nighttime catheter bag placement
|
|
A closed drainage system
should be maintained to reduce the risk of urinary tract infection. The
prevention of urinary tract infections is critical. Prevention can be
aided by using the correct hand hygiene and PPE whenever performing
catheter support.
The overnight
bag should be placed on an appropriate stand below the level of
the bladder to ensure it does not come into contact with the floor. The
leg bag should remain strapped to the person’s leg overnight to prevent it
from pulling and becoming disconnected.
Empty the contents of the
bag into the toilet. Record the amount if required.
After each use, rinse the
long-term overnight bag or re-usable leg bag with warm tap water, soak for
20 minutes in the sterilising solution, and then dry in a well-ventilated
area out of direct sunlight. When hanging to dry, place the cover over the
plastic tip on the tubing. |
|
The leg
bag is usually worn under clothing and attached to the thigh with
leg straps.
If the person uses a
wheelchair, it may be worn on the calf or hung on the wheelchair. Some
people use a drainage bag cover to maintain dignity in the
community.
The leg bag should be
emptied into a suitable container or directly into the toilet as per the
person’s choice and preference by opening the drain tap on the lower end
of the leg bag.
|
|
Ensure the catheter bag is
well anchored to the person’s leg, with extra care taken when hoisting or
transferring the person to ensure the catheter is not pulled out. Ensure
catheter bag is secured to the leg to prevent damage to the stoma, urethra
or bladder. Ensure the tubing is not kinked or twisted and the bag is
below the bladder. Poor draining may lead to infection. |
Types of Catheter Care – bag care is the same for the
different types of catheters
|
Catheter type |
Definition |
Who can insert and replace the catheter? |
Support worker responsibility |
|
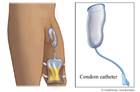
External / intermittent
catheter - male
|
Unlike other urinary catheters, a
condom catheter is not inserted into the urethra. Instead, a special
condom is attached to a catheter to keep the catheter in place and to
collect urine.
|
Trained workers can
perform this task
24 hours with a maximum of
48 hours in-between changes |
Empty catheter
bag
Keep the skin around the
catheter clean
Clean with a disposable
gauze or clean wet cloth
Report to your supervisor
if the tube is removed |
|
External / intermittent
catheter - female
|
Unlike other urinary catheters, an
external catheter is not inserted into the urethra. Instead, it is
attached to a catheter to collect urine.
|
Trained workers can
perform this task
|
Empty catheter
bag
Clean with a disposable
gauze or clean wet cloth
Report to your supervisor
if the tube is removed |
|
|
|
|
|
|
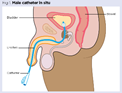
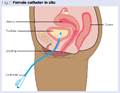
Indwelling
catheter
|
A small, flexible tube inserted through the
urethrae and into the bladder to support urine to drain.
|
Medical practitioner to
insert & replace
Change approx. every 3
months
|
Empty catheter
bag
Keep the skin around the
catheter clean
Skin care at stoma site is
required. Can become encrusted
Clean with a disposable
gauze or clean wet cloth
Report to your supervisor
if the tube is removed |
|
|
|
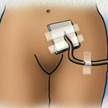
Suprapubic Catheter
(SPC)
|
The first insertion is an
invasive medical procedure where the catheter accesses the bladder
directly through the abdomen. |
Medical practitioner to
insert & replace.
Change approx. every 6 to
12 weeks |
Empty catheter
bag
If the SPC stoma site has
a discharge, report immediately to your supervisor.
Catheter becomes dislodged
report immediately to avoid the stoma closing
over |
External /
intermittent / condom catheter procedure - male
1. Wash and dry hands before
starting, apply gloves throughout process, change as
required.
2. Ensure communication and seek consent
with the participant, take all steps to ensure they are aware of what is going
to happen and communicate each step as you go along. Identify participants
preferred drainage process.
3. If necessary, remove the current condom
catheter, by rolling down the shaft of the penis (do not pull
off) if using a sealant remover, use as directed on the bottle or
tube.
4. Using a small amount of soap and water
or a medical body wipe, wipe the penis. Foreskin- gently retract and
clean the head of the penis, gently guide forward post clean
5. Rinse and gently dry until the penis is
completely dry
6. Check the shaft, head and surrounding
area of the penis for irritation or open sores. If sores or irritation
are present, complete the incident report and apply appropriate treatment as per
individual plan- pad or reapplication
7. If the catheter and participant choose
to use sealant, apply it to the skin of the penis and surrounding pubic area,
and allow it to dry- the penis should become smooth and slippery when dry.
Maintain dignity when checking, do not over-check and touch a participant more
than required.
8. Place the condom catheter over the tip
of the penis ensuring the tube area is located over the urethra, with an inch to
two inches of the tubing free. Slowly unroll, stopping at the pubic area When
using sealant, apply gentle pressure to the penis for 15 seconds to
secure.
9. Place the stealth around the base of
the penis, do not secure too tight
10. Connect the tubing to a collection bag,
ensure the connection is secure
11. Strap the drainage bag to the desired
position- drainage bad must be below the waist to support effective
drainage
12. Record the amount and consistency of urine
on the Urinary Catheter Output Chart
CCF-93
External / intermittent / wick catheter procedure –
female
1.
Check and
follow the health practitioner’s care plan
2.
Wash and dry
hands before starting, apply gloves throughout process, change as
required.
3.
Ensure
communication and seek consent with the participant, take all steps to ensure
they are aware of what is going to happen and communicate each step as you go
along. Identify participants preferred drainage process
4.
The person may prefer to lay on their back with knees bent and thighs apart or
lay on their side, frog legged
5.
Separate the legs, gluteus muscles and labia during placement and
removal.
6.
Perform perineal care, wipe with soft gauze from top to bottom and assess skin
integrity
7.
Gently tuck soft gauze side between separated gluteus and labia
8.
Ensure the top of the gauze is aligned with the pubic bone
9.
The
urethra should be aligned approximately 1/3 of the way down the length of the
product.
10.
Slowly
place legs back together once the wick external catheter is in place
11.
The anatomy holds the wick in place with most people and mesh underwear may help
secure the wick
12.
Clean the
perineum after each loose bowel movement and replace the product if
soiled.
13.
Assess
skin for compromise and perform perineal care prior to placement of a new
wick
14.
Replace
the wick after at least every 8 to 12 hours or when soiled with faeces or
blood
15.
Catheter tubing is attached to the canister or bag and emptied as per empty bag
procedure
16.
Discard
equipment and perform hand hygiene
17.
Record
the amount and consistency of urine on the Urinary
Catheter Output Chart CCF-93
In
out / intermittent catheter – male / female
Only nurses can perform this task
1.
Check and
follow the health practitioner’s care plan
2.
Wash
and dry
hands before starting, apply gloves throughout process, change as
required.
3.
Ensure communication and seek consent with the participant, take all steps to
ensure they
are aware of
what is going to happen and communicate each step as you go along. Identify
participants preferred drainage process.
4.
Participant should be placed in a comfortable sitting position.
5.
Remove in
out catheter from drawer, slightly pull back packaging with only green tubing
exposed and connect drainage bag
6.
Open remaining packaging, using no touch technique (if touched you need to throw
away and start again)
7.
Place small amount of lubricant onto the end of the tube (no touch)
8.
Collect wipes and gloves and check overnight bag is empty and not still draining
(if needed)
Participant with a vulva:
•
Instruct patient to separate the labia
majora with the non-dominant hand to expose the urethral opening, and with the
dominant hand, wash this area with warm water or moist towelettes. Start
at the top and work downwards
•
With the labia still separated by the
non-dominant hand, using the first and third fingers, the nurse uses the cotton
bud and mirror to point out the anatomy of the clitoris, urethral opening and
the vagina
•
Patient then palpates the urethra with
the second finger (feels like a small hole or donut) and leaves it over the
urethral meatus. The patient then takes the catheter in the dominant hand,
holding it two to three cm away from the tip, and gently inserts into the
urethra, sliding it under the palpating finger in a gentle upwards and backwards
motion.
Participant with a penis:
•
Instruct patient to grasp the penis at
the sides (so as not to compress the urethra) with the non-dominant
hand
•
If the patient is not circumcised,
instruct to gently retract foreskin
•
Wash the end of the penis gently with a
clean sponge or moist towelettes
• Hold the penis upright at 45/90o angle
from abdomen, grasp the catheter about 7 cm from the tip and gently insert the
catheter into the urethra until urine starts to flow.
9.
If there is an obvious urine flow, hold the catheter in place until the urine
ceases to flow.
Withdraw the catheter gently until urine recommences flowing. Once urine
flow ceases gently withdraw catheter completely.
10.
Leave the patient comfortable and lower the height of the bed.
11.
Discard equipment and perform hand hygiene.
12.
Record the amount and consistency of urine on the Urinary
In-out Catheter Output Chart CCF-97
Indwelling catheter – general care
1. Check and follow the health
practitioners care plan.
2. Check that the required equipment and
consumables are available and ready for use.
3. Confirm how the person would like to
be actively involved in their support, as outlined in their plan, and to their
chosen level.
4. Explain the procedure to the person
and seek their consent to proceed.
5. Check for any abnormalities,
including bruising, injury or skin tears
For
Female Anatomy
- Hold the end of the catheter near the
insertion site and wipe the tube with a clean,
damp cloth starting at the insertion end and working away from the urethra
(front to back).
- Clean around the urethra and labia and wipe from front to
back.
For
Male Anatomy
- Hold the end of the catheter near the
insertion site, wipe the tube with a clean,
damp cloth starting at the insertion end, and wipe from the tip of the
penis
downward.
- Start from the top of the penis where the catheter goes
in, ensuring the foreskin (if
uncircumcised) is pulled back and gently cleaned. Wipe towards the
anus.
• Gently pat the area dry with a
clean cloth.
• Secure the tubing to the leg
taking care not to kink or block it.
• Assist the person in
adjusting any clothing and making themselves comfortable.
• Check again that the tubing is
not caught in clothing, bedclothes or equipment, i.e.
wheelchair, chair,
bed.
• Remove and dispose of your
gloves and wash your hands.
• Remove the remaining PPE and
wash your hands again.
Suprapubic catheter
1. Check and follow the health
practitioners care plan.
2. Check that the required equipment and
consumables are available and ready for use.
3. Confirm how the person would like to
be actively involved in their support, as outlined in their plan, and to their
chosen level.
4. Explain the procedure to the person
and seek their consent to proceed.
5. Check for any abnormalities,
including bruising, injury or skin tears
6. Rotate suprapubic catheters daily to prevent it from
sticking to the skin (check with the health practitioner an participant
first)
7. Do
not use creams or powders on the site unless prescribed by the
doctor
8. Doctor orders to be followed for IDC
changes (nurses) and bag changes
Participants with spinal lesions at or
above T6 require
monitoring for Autonomic Dysreflexia
Symptoms:
• Severe
headache
• Sweating above the level
of the spinal cord injury
• Flushing of the
face
• Pounding in the
ears
• Blurred
vision
• Nasal
congestion
• Slow or rapid
pulse
• High blood
pressure
• Anxiety
• Headache
Action:
• call 000
• call supervisor
Contacting your supervisor / health carer
when:
• You observe skin around
the stoma site showing signs of infection or irritation
• Blocked
tubing
• Abdominal
distention
• Pain, fever
• Unusual colour or odour
to the urine
• Change in
behaviour
• Dislodged
catheter
• Skin changes
• Check in with the
participant for any concerns eg. pain or burning sensation in the bladder, lower
back pain, bladder spasms, persistent blood in urine
• Identify, document and
report information where a support plan is not meeting the participants
needs
• Support the participant
to provide feedback and request changes to their support plan as
required
Catheter care emergencies
Call 000
immediately if
• the urine output remains
unusually low, or there is no urine output
• there is persistent
blood in the urine; urine is very dark or has an offensive smell
• the person has a
temperature or complains of pain
• has a distended
abdomen
• has urine leakage around
the insertion site
• Stay calm and
collected
• Assess the situation and
seek medical attention immediately
• Call 000, your
supervisor and the health practitioner
• Record all observations
and actions in the shift notes
• Supervisors may require
an incident report form to be completed
Reporting incidents
• Write up the shift notes
during the shift, not at home in your personal time
• Report incidents to your
team leader/supervisor/supports manager and document in the shift
notes
• Your supervisor may
request an incident report form to be filled out
• In an emergency call 000
and /or your supervisor
If you
attend a shift and have a concern over the wellbeing/health of your participant,
alert the office, team leader or on-call phone straight away.
Recording observations in Carelink+ shift notes &
Urinary Catheter Output Chart
Write
timely, detailed, and accurate shift notes that relate to the catheter care
performed. This may include bag changing, recording of urine output and
consistency on the record chart and any observations.
• Write up the shift notes
during the shift, not at home in your personal time
• Urinary Catheter Output
Chart CCF-93
• Urinary In-out Catheter
Output Chart CCf-97
Documentation
Relevant documentation includes:
• Incident, Complaint, WHS
Record Form CCF-65 (supervisor will advise)
• Progress /shift notes –
Carelink+
• Urinary Catheter Output
Chart CCF-93
• Urinary In-out Catheter
Output Chart CCF-97
• Practitioners Care Plan
or Health Support Plan – Catheter Care CCF-50
• Handover
Awareness & Training
The
support worker is trained in the following skills:
• Infection control
procedures
• How to replace and
dispose of catheter bags
• How to maintain charts
and records
• How to monitor catheter
position
• How to monitor skin
condition around the catheter
• How to recognise and
respond/report blockages, dislodged catheters, signs of deteriorating
health and
infection
In
addition to the general training listed above, workers will be trained in the
specific needs of each participant they support. Training should be delivered by
an appropriately qualified health practitioner or a person who meets the
expectations of this skills descriptor.
Kyeema
should ensure that workers understand the support needs outlined in the support
plan and what risks to look for and actions required to respond to risks,
incidents, and emergencies.
Workers
are required to complete a skills review (generally annually) and participate in
participant specific training with a health practitioner. The training officer
and/or supports manager will let workers know when this will occur.
Where a
worker has not delivered this support for a period of more than three months, or
if a participant’s support needs have changed and/or they have an updated
support plan in place, it is recommended the worker be reassessed before
supporting the participant and undertake refresher training if
required.
Training provided:
Individual training plan (ITP)
• K:\Admin\Training\High
Intensity Supports ITP\Individual Training Plan
• First Aid &
CPR
Participant specific training with a healthcare
professional and the worker/s
• Participant Specific
Training Attendance Sheet HRF- 46
• K:\Admin\Training –
Participant Specific Training HISW
Sentrient online training:
• Complex Care – Catheter
Care
• Complex Care – Catheter Care
Refresher (annual refresher)
Form
used for workers to reflect and identify gaps in skills and
knowledge:
• High Intensity Supports
Skills review – Bowel & Catheter CCF-37
Responsibilities
The training officer will organise
training for the workers.
The training officer will email a monthly
reminder to team leaders to communicate any staffing and health plan
changes.
The training officer and supports
manager are responsible for ensuring workers have current skills and
knowledge, and that the training of workers is documented and regularly
audited.
• High Intensity Supports Skills
review – Bowel & Catheter CCF-37
The team leader is responsible for
updating the health support plan every year or as needed. If the plan is
unchanged after review by the speech pathologist, the team leader will add the
revised date to the plan stating that the plan is unchanged.
• Health Support Plan
– Catheter Care
CCF-50 or the health
practitioners care plan
The team leader is responsible for filing
CCF-93 on a monthly basis in the participant’s file.
• Urinary Catheter Output Chart
CCF-93 or the health practitioners
urinary output chart
The team leader is responsible for
communicating any staffing and health plan changes to the training
officer.
The support worker is responsible for
attending all allocated training sessions.
Support
workers are responsible for reporting any changes to the participants urinary
catheter, participants health and wellbeing to their supervisor.
Support
workers are responsible for reading, understanding, and signing the participants
HSP:
• Staff Acknowledgement –
Health Support Plans CCF-59
Review
and Evaluation
Support
plans are to be reviewed annually by the health practitioner. If the plan is
unchanged, the team leader will add the revised date to the plan stating that
the plan is unchanged.
The
worker supports the participant to provide feedback and request changes to their
support plan as required.
Record
Keeping
Hard
copies are filed in workers and participant files.
Electronic records are kept in participants’
file.
Training
records:
• Sentrient LMS
• Individual Training Plan
K:\Admin\Training\High Intensity Supports ITP\Individual Training
Plan
• K:\Admin\Training – Participant
Specific Training HISW (working
document)
Related Policies, Procedures and Documents:
NDIS
Practice Standards
NDIS Practice Standards:
High Intensity Support Skill Descriptors current version
Health
Support Plans
Saline & Citric Acid Flush
Recording Form CCF-13
Participant Treatment Sheet - Over-the-Counter Medication
CCF-36
High
Intensity Supports Skills review – Bowel & Catheter CCF-37
Participant Specific Training Attendance
Sheet HRF-46
Health
Support Plan – Catheter Care CCF-50
Staff
Acknowledgement – Health Support Plans CCF-59
Incident, Complaint, WHS Record Form CCF-65
Urinary Catheter Output Chart CCF-93
Urinary In-Out Catheter Output Chart CCF-97
High Intensity Supports Procedure





